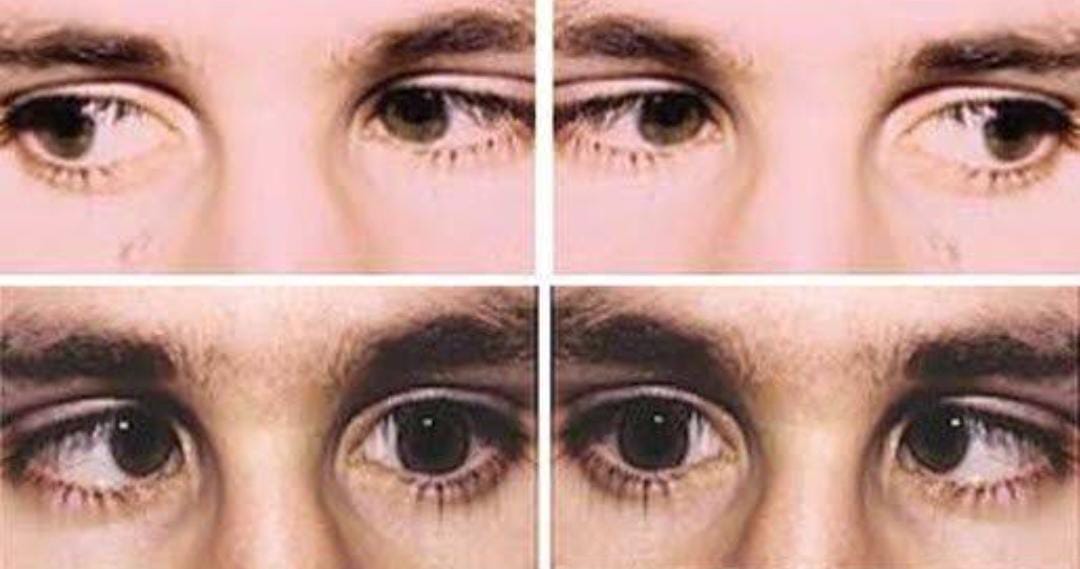
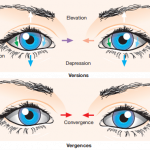
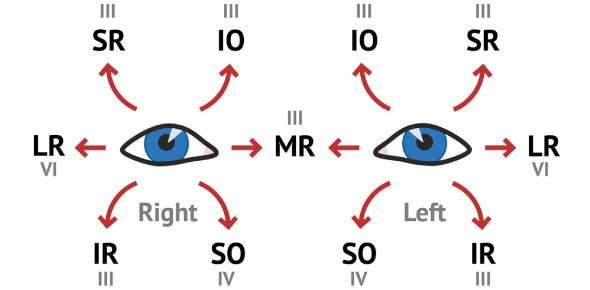
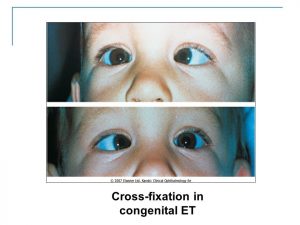
What is nystagmus?
Nystagmus is a condition that causes involuntary, rapid movement of one or both eyes. It often occurs with vision problems, including blurriness.
This condition is sometimes called “dancing eyes.”
Nystagmus is defined by rhythmic, abnormal eye movements with a “slow” eye movement driving the eye off the target followed by a second movement that brings the eye back to the target. The movement can be horizontal, vertical, torsional or a combination of these movements. Nystagmus can be jerk (named for fast phase) or pendular, variable amplitude and frequency, and can be worsened or improved by gaze position, fixation, or covering one eye (latent). This is in contrast to “saccadic intrusions” or “saccadic oscillations”, which are defined as “fast, back to back (without intersaccadic interval)” eye movements driving the eye off the visual target. The neurological origin of the saccadic intrusions/oscillations is different from that of nystagmus and is covered in a different section. In this article, different types of nystagmus, their etiologies, and treatment modalities are discussed.
Symptoms of nystagmus
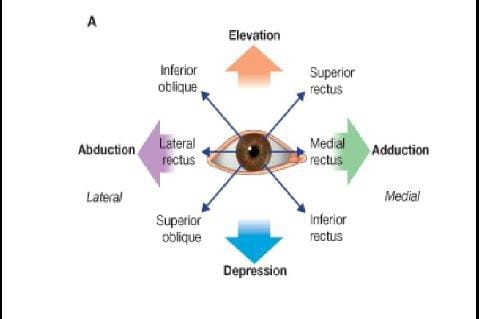
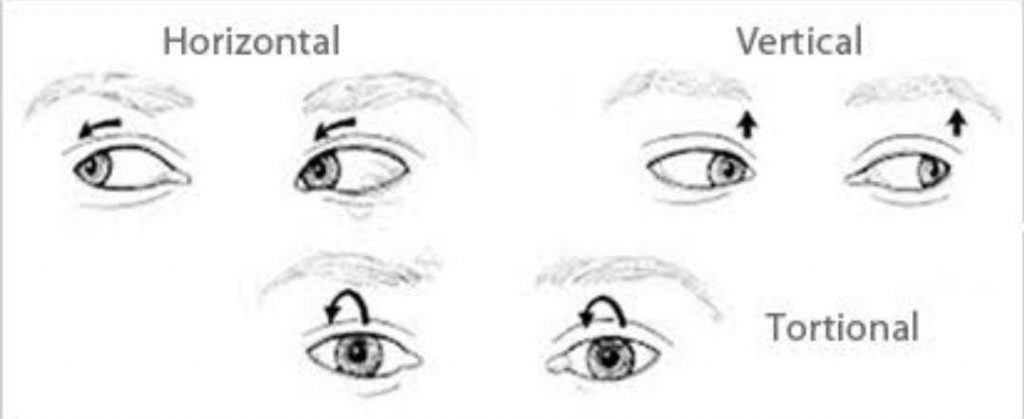
The symptoms include fast, uncontrollable eye movements. The direction of movement determines the type of nystagmus:
Horizontal nystagmus involves side-to-side eye movements.
Vertical nystagmus involves up-and-down eye movements.
Rotary, or torsional, nystagmus involves circular movements.
These movements may occur in one or both eyes depending on the cause.
Types of nystagmus
Nystagmus occurs when the part of the brain or inner ear that regulates eye movement and positioning doesn’t function correctly.
The labyrinth is the outer wall of the inner ear that helps you sense movement and position. It also helps control eye movements. The condition can be either genetic or acquired.
Infantile nystagmus syndrome
Congenital nystagmus is called infantile nystagmus syndrome (INS). It may be an inherited genetic condition. INS typically appears within the first six weeks to three months of a child’s life.
This type of nystagmus is usually mild and isn’t typically caused by an underlying health problem. In rare cases, a congenital eye disease could cause INS. Albinism is one genetic condition associated with INS.
Most people with INS won’t need treatment and don’t have complications later in life. In fact, many people with INS don’t even notice their eye movements. However, vision challenges are common.
Vision problems can range from mild to severe, and many people require corrective lenses or decide to have corrective surgery.
Acquired nystagmus
Acquired, or acute, nystagmus can develop at any stage of life. It often occurs due to injury or disease. Acquired nystagmus typically occurs due to events that affect the labyrinth in the inner ear.
Possible causes of acquired nystagmus
Possible causes of acquired nystagmus include:
stroke
certain medications, including sedatives and antiseizure medications like phenytoin (Dilantin)
excessive alcohol consumption
head injury or trauma
diseases of the eye
diseases of the inner ear
B-12 or thiamine deficiencies
brain tumors
diseases of the central nervous system, including multiple sclerosis
When to seek treatment for nystagmus
See your doctor if you begin to notice symptoms of nystagmus. Acquired nystagmus always occurs due to an underlying health condition. You’ll want to determine what that condition is and how best to treat it.
Diagnosing nystagmus
If you have congenital nystagmus, you’ll need to see an eye doctor called an ophthalmologist if the condition worsens or if you’re concerned about your vision.
Your ophthalmologist can diagnose nystagmus by performing an eye exam. They’ll ask you about your medical history to determine if any underlying health problems, medications, or environmental conditions may be contributing to your vision problems. They may also:
measure your vision to determine the type of vision problems you have
conduct a refraction test to determine the correct lens power you’ll need to compensate for your vision problems
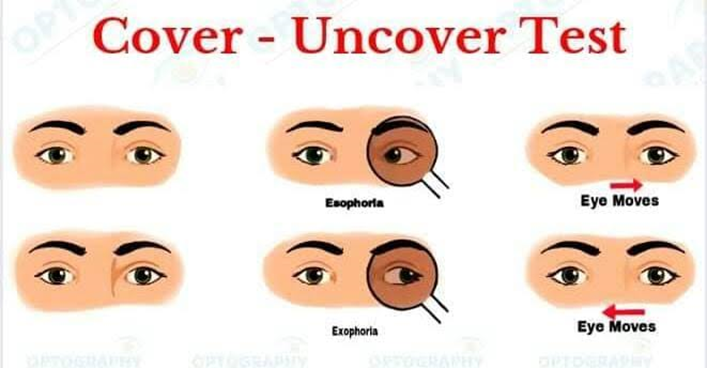
test how your eyes focus, move, and function together to look for problems that affect control of your eye movements or make it hard to use both eyes together
If your ophthalmologist diagnoses you with nystagmus, they may recommend that you see your primary care physician to address any underlying health conditions. They may also give you some tips for what to do at home to help you cope with nystagmus.
Your primary care physician can help determine what’s causing your nystagmus. They’ll first ask about your medical history and then perform a physical exam.
If your doctor can’t determine the cause of your nystagmus after taking your history and performing a physical exam, they’ll run various tests. Blood tests can help your doctor rule out any vitamin deficiencies.
Imaging tests, such as X-rays, CT scans, and MRIs, can help your doctor determine if any structural abnormalities in your brain or head are causing your nystagmus.
Treating nystagmus
Treatment for nystagmus depends on whether the condition is congenital or acquired. Congenital nystagmus doesn’t require treatment, although the following may help improve your vision:
eyeglasses
contact lenses
increased lighting around the house
[Affiliate link: magnifying devices]
Sometimes, congenital nystagmus lessens over the course of childhood without treatment. If your child has a very severe case, their doctor may suggest a surgery called a tenotomy to change the position of the muscles that control eye movement.
Such surgery can’t cure nystagmus, but it can reduce the degree to which your child needs to turn their head to improve their vision.
If you have acquired nystagmus, treatment will focus on the underlying cause. Some common treatments for acquired nystagmus include:
changing medications
correcting vitamin deficiencies with supplements and dietary adjustments
medicated eye drops for eye infections
antibiotics for infections of the inner ear
botulinum toxin to treat severe disturbances in vision caused by eye movement
special glasses lenses called prisms
brain surgery for central nervous system disorders or brain diseases
[0:42 pm, 30/12/2021] Priti Chandra Halder: Outlook for people who have nystagmus
Nystagmus may improve over time with or without treatment. However, nystagmus usually never goes away completely.
The symptoms of nystagmus can make daily tasks more challenging. For instance, those with severe nystagmus may not be able to get a driver’s license, which can limit their mobility and require them to make transportation arrangements on a regular basis.
Sharp eyesight is also important if you’re handling or operating potentially dangerous equipment or equipment requiring precision. Nystagmus can limit the types of occupations and hobbies you have.
Another challenge of severe nystagmus is finding caregiver help. If you have very poor eyesight, you may need help carrying out daily activities. If you need assistance, it’s important to ask for it. Limited eyesight may increase your chances of injury.