In pharmacology, a pharmaceutical drug, also called a medication or medicine, is a chemical substance used to treat, cure, prevent or diagnose a disease or to promote well- being.
There are different modes of administration of drugs in ophthalmology:
- Topical insitillation
- Periocular instillation
- Intraocular instillation
- Systemic administration
Topical Instillation :
They are:
– Aqueous or viscous solutions, as drops
– Ointments
– Drug impregnated contact lens
– Membrane release system (Ocusert)
Compound applied to the anterior globe surface enter the anterior chamber mainly through the Cornea. Epithelium is permeable to lipid soluble compounds and stroma to the water soluble compounds. Thus the highest intraocular concentrations following administration of compounds should be both water and lipid soluble. Epithelium being the main barrier, permeability is much increased, if the epithelium is damaged or abraded.
Eye drops: – are most popular and easy to instillate. One drop instillation is enough for each time, as the conjuctival sac cannot retain more than that. But it has a shorter duration of actions, difficult to use in children. Most of the drops get diluted by tears.
Ointments: – are particularly used in night time and also for children. Less systemic absorption via nasolacrimal duct. It also minimizes dilution, and increases contact time. Ointments cannot be used in daytime as it causes blurring of vision.
Drug impregnated contact lens : – a soft contact lens is soaked in a compound and the when the lens is placed in contact with the cornea, It gradually releases the drug e.g, pilocarpine in treatment for glaucoma.
Membrane release system (Ocusert): – provides continuous release of a predetermined amount of drug over a period of 5-7 days. Ocusert pilocarpine was available earlier for glaucoma treatment and Lacrisert ( poly vinyl alcohol) for dry eye management.
Periocular instillation:
Sub conjunctival or sub- Tenon injections are popular for administration of antibiotis, corticosteroids or atropine. This is useful at the end of intraocular operations, or treatment of corneal ulcer or iridocyclitis. A high tissue concentration is maintained for a long time.
Peribulbar or Retrobulbar blocks are used for anaesthesia.
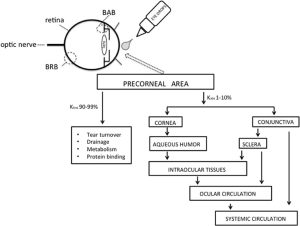
Intraocular instillation:
- a) Either into the anterior chamber (intracameral) or vitreous (intravitreal) .
- b) into the anterior chamber – in intraocular lens transplantation – e.g, visco-elastic substance, adrenaline to dilate pupil, preservative- free lignocaine for iris anaesthesia in topical phacoemulsification, pilocrapine to constrict the pupil.
Systemic administration:
Here, the drug can be given by mouth or by injections, but it has its obvious limitations due to two blood- ocular barriers: blood-aqueous barrier and blood-retinal barrier. Drugs enter the eye in proportion to their lipid solubility and smaller molecular size, e.g ; sulphonamides have much better penetration than peniclinis. Severe inflammation and trauma damage the blood-ocular barriers, and facilitate the penetration of the drugs in higher concentration.
COMMON DRUGS USED IN OPHTHALMOLOGY
ANTIBIOTICS:
Topical antibiotics: are generally required to eliminate superficial bacterial infection.
Chloramphenicol (0.5%), tetracycline(1%), ciprofloxacin(0.3%), moxifloxacin(0.5%) or gatifloxacin(0.3%) have broad spectrum effectivity.
Gentamycin(0.3%), framycetin(0.5%), tobramycin(1%) and ploymixin- B are effective against Gram ‘-ve’ bacilli.
Neomycin (0.5%) is useful only in Gram ‘+ve’ infections and cause local allergy in many cases.
Systemic antibiotics: are required to eliminate intraocular infections, and in soft tissue affections. Like cefazoline and cephalosporins have higher penetration in intraocular tissue.
Sub-conjuctival antibiotics: are best for treating deep seated infections, as high concentration is maintained in aqueous, e.g; gentamycin, amikacin, vancomycin.
Intra-ocular injections of antibiotics: either into the anterior chamber or into the vitreous, as in endophthalmitis, gentamycin, amikacin or vancomycin is usually used along with corticosteroids.
ANTIFUNGALS:
These are mainly used in keratomycosis and fungal endophthalmitis. There are three types-
- Polyenes– Amphotericin-B, nystatin and natamycin. Amphotericin-B is too toxic for sytemic use, but maybe locally used as 0.15-0.25% solution as eye drop at an interval of 1 hour. Nystatin is typically sued against Candida sp. Natamycin is used topically as 5% suspension, effective against Fusarium and Aspergillus, it is the most common antifungal.
- Imidazoles– Ketoconazole, voriconazole, fluconazole. Ketoconazole is well tolerated oral antifungal drug, Voriconazole has very good broad spectrum antifungal activity. It may be given orally (200 mg bid) or as a topical 1% preparation. Fluconazole can be used orally 200 mg daily for 3-4 weeks or 0.3% solution as 1 hourly drop in fungal corneal ulcer.
- Flucytosine- 5-fluorocytosine.
ANTIVIRALS:
Ocular viral infections is mainly concerned with keratitis caused by Herpes simplex virus and also to some extent by Herpes zoster . Acyclovir is effective both topically and systemically. It is used as 3% ointment or oral tablets in herpes simplex keratitis.
AUTONOMIC DRUGS:
Autonomic drugs act on sphincter and dilator pupillae muscle of iris and also on the ciliary muscle. They are Miotics, Mydriatics and Cycloplegics.
Miotics: they cause papillary constrictions. Pilocarpine is the most commonly used miotic.almost in glaucoma cases miotics are used.
Mydriatics: pupil dilating drugs are called mydriatics. They all dilate the pupil and also causes paralysis of cliary muscle in greater or lower degree. Atropine (1%), Homatropine(1-2%), Cyclopentolate(0.5-1%) make it impossible for the sphincter papillae muscle to contract. Wheres Adrenaline as intra-cameral injection act on the dilator papillae directly. Atropine is the strongest cycloplegic agent and its effect lasts for 10-14 days. They are mainly used for fundus examination,for preoperative assessment of cataract, during posterior chamber surgery. Cycloplegics are mainly used for refraction in children.
OCULAR HYPOTENSIVE:
The drug causing the lowering of intra ocular pressure, are called ocular hypotensives. There are two types:
Systemic: acetazolamide 250 mg as tablets 1-2 tabs 4 times daily, Ethoxzolamide, Methazolamide, Inj. Mannitol is administered intra-venously.
Local: Pilocarpine(1-4%) eye drop, Timolol maleate(0.25-0.5%), Betaxolol(0.50%). Ocular hypotensives may be used alone or in combination depending upon the height of intraocular pressure.
LOCAL ANAESTHETICS:
The small size of the eye and the accessibility of its nerve supply permit most adult ocular surgeries to be done under local ansethesia. There are two types: Topical and Infiltrative.
Topical: they work by stabilizing the nerve membrane potential temporarily. Lignocaine hydrochloride 2%, Proparacaine 0.5%.
Infiltrative: simultaneous motor and sensory block are obtained in infiltrative anesthesia in and around the eyeball. For infiltration Lignocaine 2% is normally used. Bupivacaine 0.5% is a long acting anesthetic agent is usually mixed with lignocaine (50:50) to achieve better and prolonged anaesthetic effect.
CORTICOSTEROIDS:
The corticosteroid reduces the inflammation of the ocular tissues by-
– decreasing capillary permeability
– limiting exudation
– inhibiting the formation of new and granular tissues.
Hydrocortisone has the weakest power followed by Prednisolone, Dexamethasone, Betamethasone in increasing efficiency. It can be used locally as drops, sub Tenon or sub- conjunctival injections, retrobulbar injections. Systemically it is used by intra-muscular in severe iridocyclitis or pseudotumour of the orbit.
NON-STEROIDAL ANTI-INFLAMMATORY DRUGS:
As the corticosteroids have many complications, these days some non-steroidal anti-inflammatory drugs are being used, such as Flurbiprofen sodium, Diclofenac sodium, Bromfenac, Nepafenac (it has the best corneal and intraocular penetration).
VISCO- ELASTIC SUBSTANCE:
These are tissue protective visco elastic substance molecular weight ranging from 30000 to 4 million dalton. They are non-toxic, non antigenic and do not interfare normal wound healing. It protects corneal endothelial cell, maintains anterior chamber depth during intra-ocular surgeries. Sodium Hyaluronate 1%, Methyl Cellulose 2%, Hydroxypropryl methyl cellulose (HPMC).
These are types of drugs mainly used in ophthalmology.