With the rapid development in electronics and micro computers a number of innovative methods & instrument for automated clinical refraction have appeared since 1960.
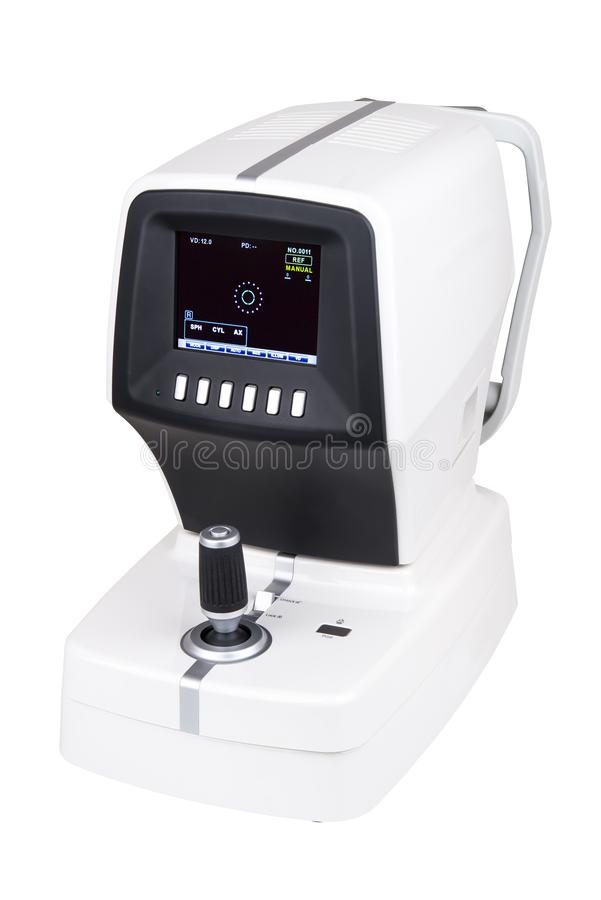
Refractometer is used to determine the degree of ametropia with the use of optometers and automated refractometers.
Modern automated refractors give according to same quite accurate readings but in the experience of the author such is not the case . Automated refractor. However, provides enough guidelines for the accurate measurement of ametropia in a patient. Most of the automated refractors utilise infrared light source. The measurement depend on
1.Scheiner’s double pinhole method
2.Retinoscopic illumination system
3.A grating principle
SCHEINER’S PRINCIPLES:-
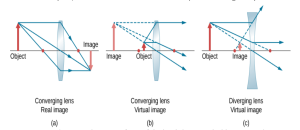
In 1619,scheiner discovered that the point at which an eye is focused could be precisely determined by placing double pinhole apertures before the pupil. The two pinhole apertures limit the rays of light to two small bundles. If the eye is myopic, the ray bundles cross each other before focusing on the retina and two small spots of light are seen. In a hypermetropic eye, however, the ray bundles are interrupted by the retina before they meet and again two small spots of light are seen. The two pints of light coalesce to a single point when the object as moved to the far point of the eye. In this manner, the refractive error of the eye can be determined. The end point of singleness is more precise than the judgment of least blur.
Modern autorefractometers:-
Automatic refractometers automatically measure the refractive index of a sample. The automatic measurement of the refractive index of the sample is based on the determination of the critical angle of total reflection. A light source, usually a long-life LED, is focused onto a prism surface via a lens system. An interference filter guarantees the specified wavelength. Due to focusing light to a spot at the prism surface, a wide range of different angles is covered. As shown in the figure “Schematic setup of an automatic refractometer” the measured sample is in direct contact with the measuring prism. Depending on its refractive index, the incoming light below the critical angle of total reflection is partly transmitted into the sample, whereas for higher angles of incidence the light is totally reflected. This dependence of the reflected light intensity from the incident angle is measured with a high-resolution sensor array. From the video signal taken with the CCD sensor the refractive index of the sample can be calculated. This method of detecting the angle of total reflection is independent on the sample properties. It is even possible to measure the refractive index of optically dense strongly absorbing samples or samples containing air bubbles or solid particles . Furthermore, only a few microliters are required and the sample can be recovered. This determination of the refraction angle is independent of vibrations and other environmental disturbances.
Limitations of autorefractometers:-
1.The individual patient can accommodate to the instrument.
2.Reflection over the patient’s current glasses can occur.
3.Some autorefractometers do not provide vision as an end point. Consequently, if there is an error in the printout., the examiner does not know if the measurement is reliable.
4.Peripheral light from the room can affect the reading, thus a dark chamber is required.
Why this Modern Refractometers needed?
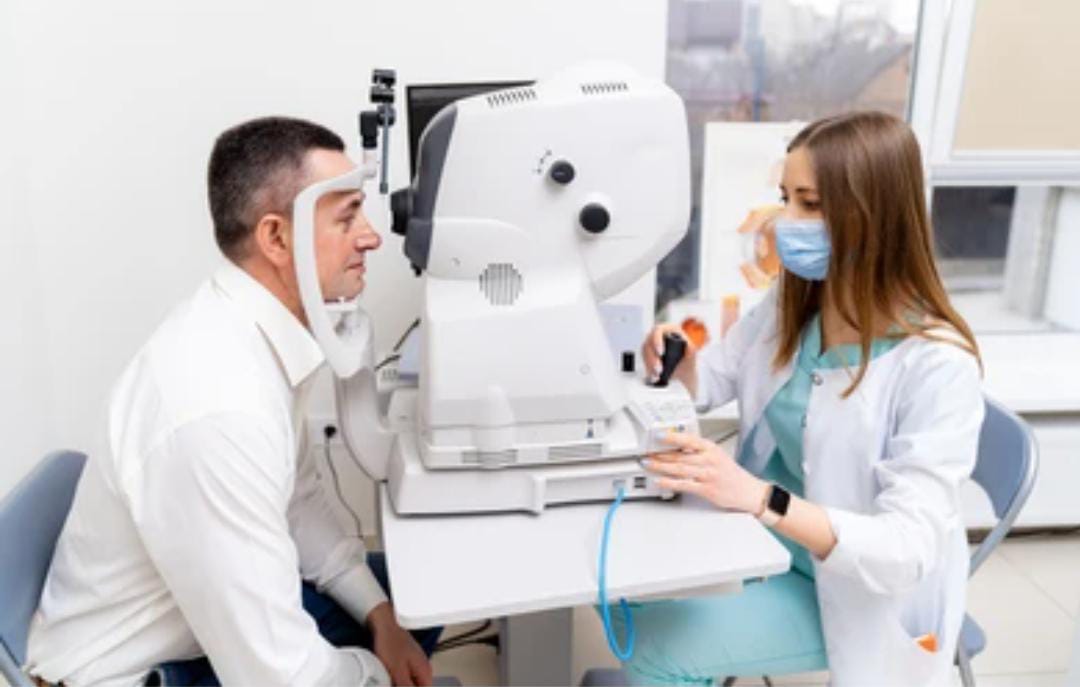
•The reason for its increasing popularity is primarily that automated refraction devices offer speed, reasonable accuracy and repeatability.
•With the increasing load of patients in any ophthalmology or optometrist in practice. The practioners are focused with the challenge of completing all tasks within a fixed time frame. An autorefractometers will, therefore increase the speed and efficiency of the refraction process.