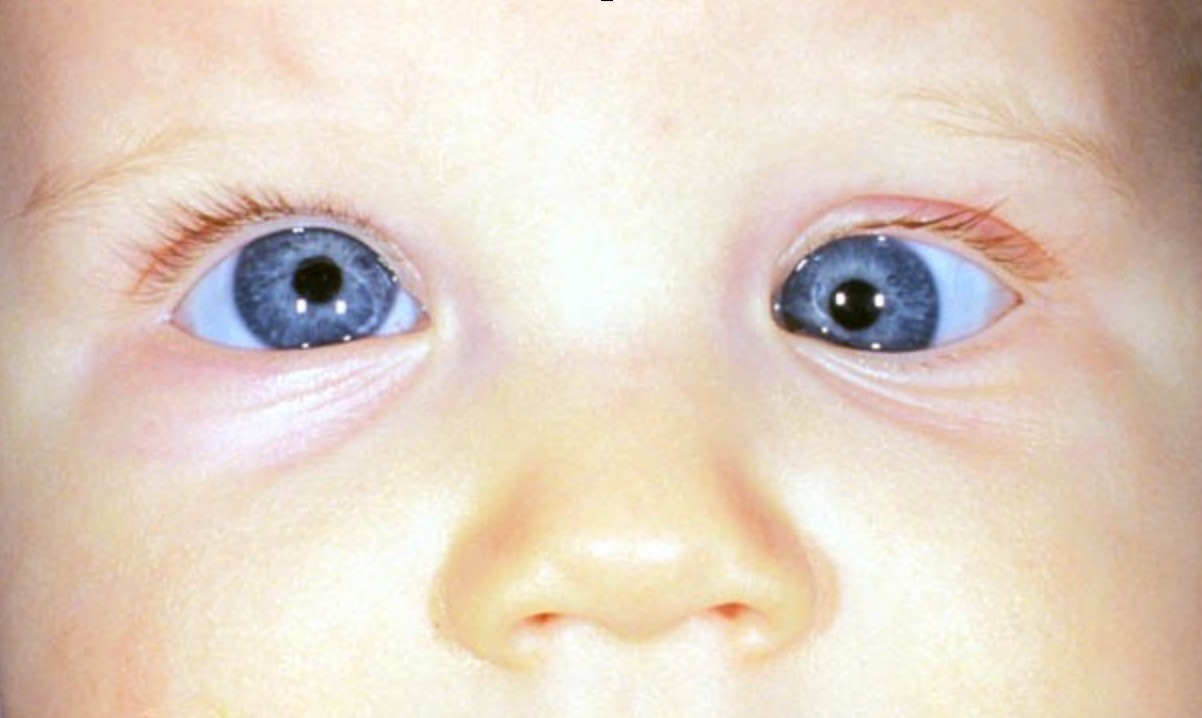
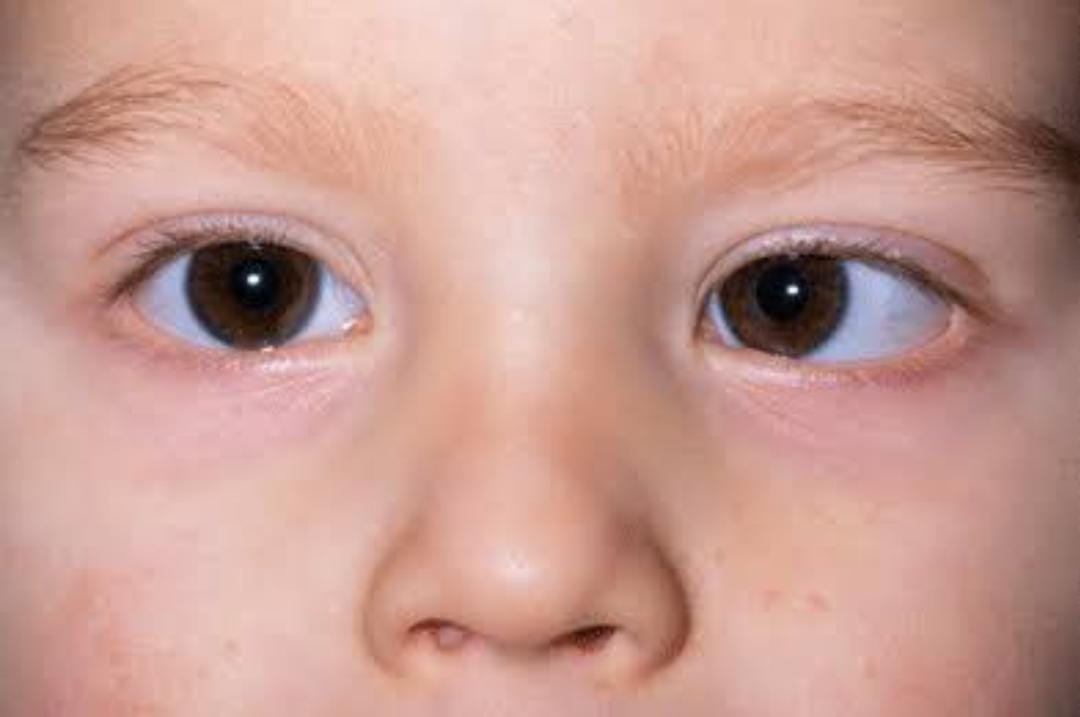
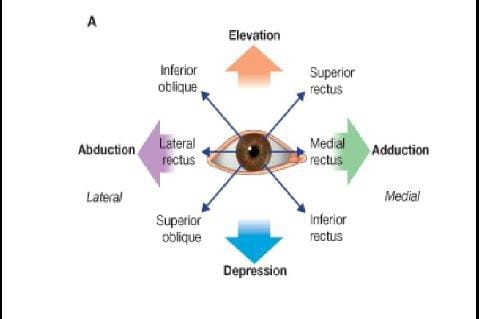
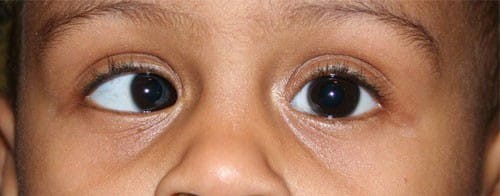
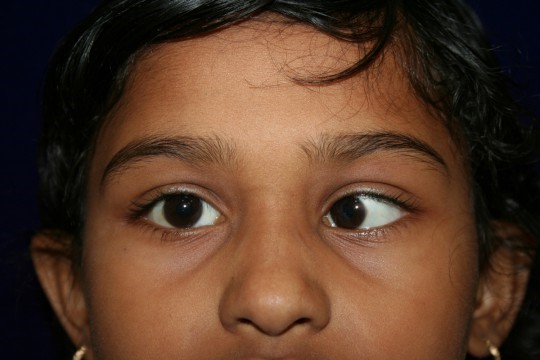
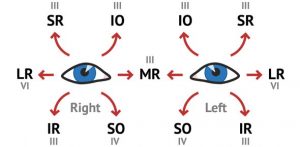
STRABISMUS:- Normally, visual axis of the two eyes are parallel to each other in the primary position of gaze and this alignment is maintained in all positions of gaze.
A misalignment of the visual axes of the two eyes is called squint or strabismus.
HISTORY OF PATIENTS-
Before examination the patient’s eye a careful history of ocular complaints should be taken.
•Name, Age, Gender, Address and occupation of the patient.
∆Chief presenting complaints of the patient:-
•Dimness of vision
•Redness
•Watering and itching of the eyes
•Sudden loss of vision
•Dimness of vision a particular time.
•Abnormal deviation of the eyeball.
•Headeche
•History of any injury
•Photophobia
•Diplopia
•Is the deviation constant or intermittent?
•Is the deviation present for distance, near or both?
•Is it unilateral or bilateral?
•Is it present only when the patient is inattentive or fatigued?
•Is it associated with trauma or physical stress?
∆Past History:-
•Any ocular trauma
•Wearing of spectacle
•Similar problem in the other eye.
•Birth history (are it’s premature baby)
∆Operative history:-
•Any operation on the same eye or opposite eye or both eye. Name and date of operation or old prescription.
•Duration of hospital stay at that time
•Any known operative complications.
∆Medical history including medication:-
•Diabetes, hypertension
•Bronchiol asthma
•Tuberculosis
•Tobacco, alcohol
•Acidity, heart burn
•Drug history including drug allerrgy.
VISION EVALUATION-
IT’S most important, because a refractive error may be responsible for the symptoms of the patient or for the deviation itself.
∆Visual acuity Test – Each eye should be tested separately and then binocularly.
∆Visual Acuity with PIN HOLE – Same, Each eye should be tested separately and then binocularly And note it how much vision improved compare to normal visual acuity.
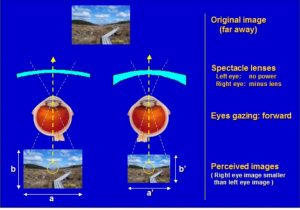
∆Determination of refractive error-
Hypermetropia, myopia, anisometropia and astigmatism may all be associated with strabismus. To find out refractive error refraction should be performed under full cycloplegia, especially in children.
•Cycloplegia:-The commonest refractive error causing strabismus is hypermetropia. Accurate measurement of hypermetropia necessitate effective Paralysis of the ciliary muscle, in order to neutralize the effect of accommodation, which masks the true degree of this refractive error.
1) CYCLOPENTOLATE:-It affords cycloplegia in most children. The concentration employed is 0.5% under the age of 6 months and 1% there after. One drop, repeated after 5 minutes, usually results in maximal cycloplegia within 30 minutes, with recovery of accommodation within 2-3 hours and of mydriasis within 24 hours.
2) ATROPINE:-
•It may be necessary in children in some children with either high hypermetropia or heavily pigmented irides, in which cyclopentolate may be inadequate.
• Atropine may be used as drops or ointment. Drops are easier for an untrained person to instill but there is less risk of overdose with ointment. The concentration is 0.5% under the age of 12 months and 1% thereafter.
• Maximal cycloplegia occurs at 3 hours. Recovery of accommodation strats after about 3 days and is usually complete by 10 days.
•Atropine is instilled for 3 days before retinoscopy but not on the day of examination. The parents should be warned do discontinue medication if there are signs of systemic toxicity.
∆Change of Refraction:-
•Refraction changes with age, it’s important to check atleast every year and more frequently in smaller children and if acuity is reduced.
•At birth most babies are hypermetropic.
•After the age of 2 years there may be an increased in hypermetropia and decrease in astigmatism.
∆Fundas Examination:-
Fundas examination should be emphasized that dilated fundoscopy is mandatory in the context of strabismus , to exclude any underlying ocular pathology such as muscular scarring, optic disc hypoplasis or retinoblastoma.
∆Pupilary reaction:- Pupilary reaction helps to differential primary deviation from secondary, i. e paralytic squint with non paralytic.