Strabismus and amblyopia are frequently confused with each other, and people often use the terms interchangeably. They are, in fact, two different eye conditions, albeit with some shared characteristics. Put simply, strabismus is a problem with the alignment of the eyes and is informally called “crossed eyes”. The eyes do not look in the same direction at the same time, as they should. Amblyopia, however, is essentially a problem with a person’s eyesight. It’s also known as a “lazy eye” and typically means that they cannot see an image clearly in one (or sometimes both) of their eyes. Strabismus and amblyopia are functional vision problems, stemming from issues with how the eyes work together, known as “eye teaming”. In most cases, there are also problems with areas of eye focusing and eye movement, highlighting issues between the eyes, brain and visual pathways.
STRABISMUS :
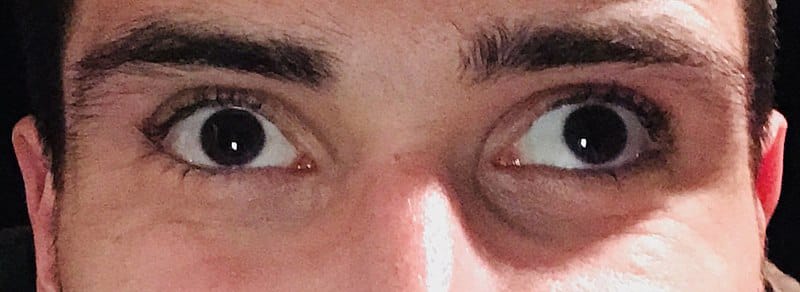
Strabismus (crossed eyes) is a condition in which the eyes do not line up with one another. In other words, one eye is turned in a direction that is different from the other eye.
Under normal conditions, the six muscles that control eye movement work together and point both eyes at the same direction. Patients with strabismus have problems with the control of eye movement and cannot keep normal ocular alignment (eye position).
Strabismus can be categorized by the direction of the turned or misaligned eye:
- Inward turning (esotropia)
- Outward turning (exotropia)
- Upward turning (hypertropia)
- Downward turning (hypotropia)
CAUSE :
Most strabismus results from an abnormality of the neuromuscular control of eye movement. Our understanding of these control centers in the brain is still evolving. Less commonly, there is a problem with the actual eye muscle. Strabismus is often inherited, with about 30 percent of children with strabismus having a family member with a similar problem.
Other conditions associated with strabismus include:
- Uncorrected refractive errors
- Poor vision in one eye
- Cerebral palsy
- Down syndrome (20-60% of these patients are affected)
- Hydrocephalus (a congenital disease that results in a buildup of fluid in the brain)
- Brain tumors
- Stroke (the leading cause of strabismus in adults)
- Head injuries, which can damage the area of the brain responsible for control of eye movement, the nerves that control eye movement, and the eye muscles
- Neurological (nervous system) problems
Graves’ disease (overproduction of thyroid hormone)
TYPES :
Many types of strabismus can develop in children or adults, but the two most common forms are below.
Accommodative esotropia
Accommodative esotropia often occurs because of uncorrected farsightedness (hyperopia). The eye’s focusing system is linked to the system that controls where the eyes point. People who are farsighted are focusing extra hard to keep images clear. This may cause the eyes to turn inward. Symptoms of accommodative esotropia may include seeing double, closing or covering one eye when doing close work, and tilting or turning the head.
Intermittent exotropia
Intermittent exotropia may develop when a person cannot coordinate both eyes together. The eyes may point beyond the object being viewed. People with intermittent exotropia may experience headaches, difficulty reading and eye strain. They also may close one eye when viewing at distance or in bright sunlight.
Symptoms
Symptoms of Strabismus include:
- Eyes that look misaligned.
- Eyes that do not move together.
- Frequent blinking or squinting,especially in bright sunlight.
- Tilting the head to look at things.
- Faulty depth perception
- Double vision.
HOW STABISMUS AFFECT ON NORMAL VISION ?
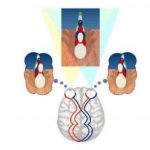
With normal vision, both eyes aim at the same spot. The brain combines the two images from our eyes into a single, three-dimensional (3-D) image. This is how we can tell how near or far something is from us (called depth perception).
When one eye is out of alignment, two different pictures are sent to the brain. In a young child, the brain learns to ignore the image of the misaligned eye. Instead, it sees only the image from the straight or better-seeing eye. As a result, the child loses depth perception.
Adults who develop strabismus after childhood often have double vision. This is because their brains have already learned to receive images from both eyes. Their brains cannot ignore the image from the turned eye, so they see two images.
DIAGNOSIS :
- Patient history (to determine the symptoms the patient is having, family history, general health problems, medications being used and any other possible causes of symptoms)
- Visual acuity (reading letters from an eye chart, or examining young children’s visual behavior)
- Refraction (checking the eyes with a series of corrective lenses to measure how they focus light). Children do not have to be old enough to give verbal feedback when checking for glasses.
- Alignment and focus tests
- Examination after dilation (widening) of the pupils to determine the health of internal eye structures.
TREATMENT :
strabismus (crossed eyes) surgery
This is the most common treatment for strabismus. Surgery can improve eye alignment and help restore proper vision.
Typically, strabismus occurs when the muscles around the eyes are either too stiff or too weak. An ophthalmologist can loosen, tighten, or move certain eye muscles so that the eyes line up properly to work together. More than one surgery may be needed to treat strabismus.
Surgery :
Surgery is usually done as outpatient surgery in a hospital or surgery center, using either general or local anesthesia. There makes a small cut in the tissue covering the eye to reach the eye muscles. The muscles are then repositioned to help the eyes point in the same direction. This may need to be done in one or both eyes. After strabismus surgery, you can get back to your daily routine within a few days.
Eye muscle exercises
Eye exercises to help you focus both eyes inward. These exercises can help if you have “convergence insufficiency.” That is when your eyes do not align properly for close tasks, like reading or computer work.
EYEGLASSES / CONTACT LENSES :
Eyeglasses or contact lenses used in patients with uncorrected refractive errors. With corrective lenses, the eyes will need less focusing effort and may remain straight.
Prism eyeglasses
A prism is a clear, wedge-shaped lens that bends (refracts) light rays. A prism can be attached to eyeglasses or made as part of the lens. Prisms can help some people with mild double vision see one image, not two.
Botulinum toxin (Botox)
In some cases, an injection (shot) of this drug in the eye can help treat strabismus. It paralyzes the muscles that keep your eyes from aligning properly. The effect can last for just a few months, or it could permanently improve eye
AMBLYOPIA :
A lazy eye is when the vision of one of your eyes doesn’t develop the way it should. It’s also call this amblyopia.
Without treatment, your brain will learn to ignore the image that comes from the weaker eye. That could cause permanent vision problems.
SIGNS OF LAZY EYE :
Amblyopia starts in childhood, usually between ages 6 and 9. Identifying and treating it before age 7 brings the best chances of fully correcting the condition.
Common symptoms include:
- Trouble telling how near or far away something is (depth perception)
- Squinting or shutting one eye
- Head tilting
- Clumsiness
- Eye strain
- Fatigue with near work
CAUSES :
Refractive errors: These conditions affect how light passes through the eye. They include:
- Nearsightedness (myopia), trouble seeing far away.
- Farsightedness (hyperopia), trouble seeing up close.
- Astigmatism, a curved cornea.
Strabismus (crossed eyes): The eyes are meant to move together as a pair, but sometimes they don’t. If one drifts (in, out, up or down), the brain may rely on one eye over the other, leading to amblyopia.
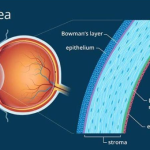
Structural problems : Sometimes, the eye has a structural problem that can lead to amblyopia, including:
- Cataracts, which cause cloudiness in the lens and blurry vision.
- Astigmatism.
- Droopy eyelid.
- Scar on the cornea.
TYPES :
All three types of amblyopia result from suppression of vision in one or both eyes. The difference is in the root cause of the suppression.
- Refractive amblyopia: Results from an uncorrected high prescription in one or both eyes.
- Strabismic amblyopia: Results from a constant eye turn in one eye.
- Deprivation amblyopia: Results from impaired vision in one eye due to physical problems in the eye.
HOW AMBLYOPIA AFFECT ON CHILD ?
In a child with amblyopia, one eye has blurred vision, and the other has clear vision. The brain begins to ignore the blurry eye and uses only the eye with clear vision. Eventually, the brain learns to rely on the stronger eye, allowing the weaker eye to worsen.
RISK FACTORS :
- Some children may have risk factors for amblyopia, including:
- Family history of eye problems.
- Developmental disabilities.
- Born early (premature birth).
- Small at birth.
DIAGNOSIS :
- Put drops in the eye to make the pupil bigger.
- Shine a light in each eye.
- Cover one eye at a time and test whether each eye can follow a moving object.
- Ask older children to read letters on a chart on the other side of the room.
Treatment :
Amblyopia treatment is much more effective if it starts early, while the connections between the eyes and brain are still developing. Strategies focus on making the child’s brain use the weaker eye. Options include:
Eye patches for kids: Your child may wear a patch over the better eye for at least a few hours per day. This effective treatment can last months or even years. The patch forces the brain to use the images from the weaker eye, eventually making that eye stronger.
Glasses: Eyeglasses are also a common lazy eye treatment. They can help amblyopia by improving nearsightedness, farsightedness and eye crossing.
Eye drops: For mild cases, your provider may recommend eye drops (atropine) to temporarily blur vision in the better eye. The goal is the same as a patch: to force the brain to use the weaker eye.
Surgery: An operation for amblyopia is rare. Your healthcare provider may suggest surgery to fix certain causes of amblyopia, such as cataracts.
PSYCHOLOGICAL ADAPTATION :
Ignoring is a psychological adaptation which is learnt by some visually matire patients to deal with the annoying diplopia. It probably falls somewhere b/w conscious and unconscious thought. All patients cannot learn to ignore diplopia. Further, it has also been reported that the patients with excellent acuity in each eye may be able to ignore the weaker image while the patients with poor vision cannot. Hoe this occurs is not known exactly. Perhaps the individual’s psychologic factors play an important role in the development of rare phenomenon of ignoring.