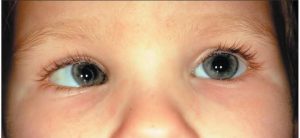
Everybody knows about cataract .And most of the people think that cataract happen only to aged people . But it is not true nowadays. Cataracts can be seen in the children too. In children the cataract is called paediatric cataract. This type of cataract can be congenital or acquired.
What is cataract ?
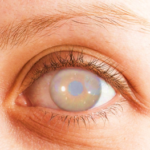
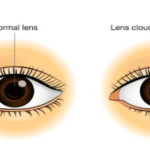
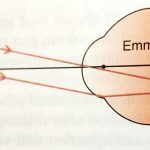
“Cataract” word has been derived from the greek word “katarraktes” which means waterfall. A cataract is a clouding of the eye. It can happen at any age. The crystalline lens should be clear, so that the light rays can reach the retina.
In adult the type of cataract is developmental,traumatic etc. But in children’s eyes and brains are being developed till the age of 8 or 10 years. That’s why untreated cataracts can be severe, permanent effects on their vision.
Types of cataract in children
- Congenital or acquired
- Genetics
- Diabetes
- Traumatic
Etiology
The congenital cataract has no identifiable cause. The fifteen genes are responsible to make cataract and the inheritance is most autosomal dominant or x linked or aautosomal recessive. Some systemic disease such as galactosmia, hypocalcemia and diabetes. Some infections like rubella, herpes simplex, toxoplasmosis,varicella,syphilis. Trauma is a well known cause of paediatric cataracts.
Cataracts seen in children
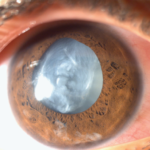
Blue dot cataract
This is one of the most common type of congenital cataract.It usually forms in the first two decades of life .Opacities are usually stationary and do not affect vision.
Rubella Cataract
Maternal Rubella infection happened during first trimester (second and third month) may cause rubella cataract.In this case the child’s eye is pearly white nuclear cataract. Lens matter may remain soft or may even liquify (congenital Morgagnian cataract).
But the congenital rubella cataract can be prevented by vaccination of the mother. Since the rubella vaccine is toxic to foetus, it must therefore, be administered atleast three months before the pregnancy.
Congenital Membranous Cataract
Some times there may occur total alone or as partial absorbtion of congenital cataract.Total lens fibre are disappeared and transparent lens capsule remains behind .This is associated with Hallermann Streiff Francois Syndrom.
Diagnosis
Slit lamp Biomicroscopy
Intra Ocular Pressure
Family History should be required. In case without clear family history , a total paediatric and developmental exam should be performed.
Some lab works including Torch titers, VDRL, serum calcium and phosphorus levels.
Signs
Easily visible opacity in the lens.
Microcornea
Megalocornea
Coloboma of the iris, aniridia, and zoniular dehiscence.
Symptoms
Lack of reaction to light.
Strabismus
Photophobia
Nystagmus
Treatment
Non surgical
Observation with careful regular monitoring to look for any change or progression in cataract or development of amblyopia. If either occurs treatment is recommended.
Pharmacologic papillary dilation can be used to increase the pupil size and allow the child to see through a clear portion of the lens. Cycloplegic drops should be avoided as they can cause loss of accommodation and can lead to amblyopia.
Occlusion of the other eye is useful in case of unilateral cataract to prevent amblyopia until surgery is completed.
Surgical
Any cataract that is visually significant >3 mm central opacity , centrally obscuring posterior pole, with strabismus or nystagmus. SICS technique should be done. Lens aspiration should be combined with primary posterior capsulotomy in children below 6 years of age and also with anterior vitrectomy in all children below 2 years of age.
Complications
Wound leakage
Vitreous incarceration
IOL capture
Post opertative inflammation
Post operative increased IOP
Vitreous haemorrhage
Retinal haemorrhage
Retinal detachment
Post operative endopthalmitis
References
Dr A K Khurrana Comprehensive Ophthalmology
Must knows in Ophthalmology- Prof Sambuddha Ghosh
Eyewiki.aao.com
American Academy of Ophthalmology